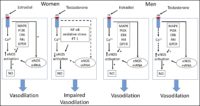
Sex differences in the signal transduction pathways of endothelial nitric oxide (NO) synthase (eNOS) activation in endothelial cells by estradiol and testosterone and the subsequent vascular response. Estradiol is generally thought to increase NO availability through genomic and nongenonimc pathways in both men and women, resulting in vasodilation. Testosterone has similar effects in men. Testosterone works through a separate pathway in women, resulting in reduced NO availability and impaired vasodilation. The dashed line indicates effects that are uncertain. ER, estrogen receptor; AR, androgen receptor; PI3K, phosphatidylinositol 3-kinase; GPER, G protein-coupled estrogen receptor 1.
Dr. Nina Stachenfeld’s paper describing sex differences in cardiovascular function and risk across the lifespan was just released in the December 2018 issue of The American Journal of Physiology. Congratulations to Dr. Stachenfeld and her colleagues, Dr. Anna Stanhewicz and Dr. Megan Wenner.
Abstract – Diseases of the cardiovascular system are the leading cause of morbidity and mortality in men and women in developed countries, and cardiovascular disease (CVD) is becoming more prevalent in developing countries. The prevalence of atherosclerotic CVD in men is greater than in women until menopause, when the prevalence of CVD increases in women until it exceeds that of men.
Endothelial function is a barometer of vascular health and a predictor of atherosclerosis that may provide insights into sex differences in CVD as well as how and why the CVD risk drastically changes with menopause. Studies of sex differences in endothelial function are conflicting, with some studies showing earlier decrements in endothelial function in men compared with women, whereas others show similar age-related declines between the sexes. Because the increase in CVD risk coincides with menopause, it is generally thought that female hormones, estrogens in particular, are cardioprotective. Moreover, it is often proposed that androgens are detrimental. In truth, the relationships are more complex.
This review first addresses female and male sex hormones and their receptors and how these interact with the cardiovascular system, particularly the endothelium, in healthy young women and men. Second, we address sex differences in sex steroid receptor-independent mechanisms controlling endothelial function, focusing on vascular endothelin and the renin-angiotensin systems, in healthy young women and men. Finally, we discuss sex differences in age-associated endothelial dysfunction, focusing on the role of attenuated circulating sex hormones in these effects.

